How to Treat 10 Common Skin Concerns That Need to Be Normalized


Recently, I was having a conversation with a couple of co-workers via Slack about dandruff and then about the skin-chafing situation currently happening between our thighs and then the random breakouts summer sweat and sand have so kindly sprinkled every which way from boob to bum. And then it hit me. Despite the vast number of products that do indeed exist to help manage, treat, and prevent such common skin conditions like the above, we don't ever really talk about them. I mean, God forbid we actually discuss said dandruff, thigh chafe, and shaving-induced pustules on the internet. The horror, right? Hopefully, you can detect my sarcasm here.
Sure, it's sexy to discuss the glow-enhancing serums that instantaneously impart epic skin luster or the body oils that drench our limbs with a sun-induced gleam, but common skin conditions like melasma, folliculitis, seborrheic dermatitis (an inflamed version of dandruff), and heck, even cold sores unfairly retain a hush-hush layer of stigma. So let's address it, shall we? Even though we might not be openly chatting about the skin conditions that make us boil, scale, or pigment, many—let me repeat, many—of us experience them, and it's high time we work harder to talk about and normalize them.
Since summer is prime time for all things to go especially funky where skin conditions are concerned (whether said conditions develop or worsen), I consulted three top dermatologists to lend their professional intel. Below, we're covering 10 common skin conditions—what they are, how they present, what causes them or makes them worse, and last but not least, how to manage or treat them. Keep scrolling!
Dandruff/Seborrheic Dermatitis
What is it, and what causes it? According to New York–based dermatologist, Joshua Zeichner, MD, dandruff is the redness and flaking of the skin which occurs (most often) on the scalp but can also manifest in other areas like the eyebrows, ears, smile lines, and even the chest. It can be itchy and uncomfortable, and it's thought to be caused by high levels of yeast on the skin, which can lead to an uptick in inflammation.
While experts don't exactly know why, some people are genetically more predisposed to react to yeast than others, and dermatologist and dermatologic surgeon Michelle Henry, MD, points out that almost half of Americans will suffer from dandruff at some point in their life. "Dandruff is not a disease of poor hygiene," she confirms right off the bat. "People with seborrheic dermatitis—a condition that is more severe than regular dandruff, which is uninflamed—are more likely to have dandruff."
What makes it worse? "Seborrheic dermatitis tends to get worse in warm, humid months or after exercise when the skin sweats more and oil becomes trapped on the skin," Zeichner explains. "This creates an environment that allows yeast to grow to high levels."
Additionally, Henry says excessive shampooing or, conversely, not shampooing often enough; products that cause irritation; underlying health conditions; diet; and stress may also potentially exacerbate both scalp conditions.

How to deal: As far as treating and managing the condition and its symptoms, Zeichner cites dandruff treatments containing antifungal medications as one of the best treatment options. These medications help lower yeast levels on the skin and, in effect, also reduce inflammation.
"Dandruff is not a true infection, and it is not contagious," Zeichner confirms. "If you have thick flaking, consider a salicylic acid–containing shampoo to help exfoliate dead cells and flakes, such as Neutrogena's T/Gel Therapeutic Shampoo. Remember that the treatment is for your scalp, not your hair. Rub the shampoo into the scalp, and let it sit while you apply your regular shampoo onto the hair. Then rinse both out together."
In addition to salicylic acid, Henry says to look for anti-dandruff shampoos that also contain strategic ingredients such as sulfur, tar, zinc pyrithione, and selenium sulfide. "Neutrogena's T/Sal Therapeutic Shampoo for Scalp Build-Up is a good choice that is a three-in-one formula targeted to treat dandruff, seborrheic dermatitis, and psoriasis. Another option is Neutrogena's Healthy Scalp Clarify & Shine Shampoo and Conditioner. Both are free of chemicals that could further aggravate your scalp and gently exfoliate with alpha hydroxy acid from grapefruit," she says.
Chafing
What is it, and what causes it? As Zeichner explains, chafing is essentially inflammation of the skin caused by friction. Said friction disrupts the outer skin layer and causes loss of hydration and irritation. The skin becomes red and inflamed, and it's often associated with an uncomfortable burning sensation that can (if severe enough) lead to blisters or raw, open skin. "It's a common skin problem for people of all skin types, shapes, and sizes," confirms Henry.
What makes it worse? Exercise, sweating, heat/humidity, rough fabrics, and constrictive or tight clothing. According to Zeichner, chafing most often occurs wherever skin is rubbing on skin (like between the thighs), and it's especially common after exercise when there might be an increase in friction.

How to deal: "Wear loose-fitting clothing and make sure you keep your skin well moisturized," says Zeichner. "Prioritize petrolatum-based moisturizers like Vaseline Petroleum Jelly for irritated skin, and if needed, apply an over-the-counter 1% hydrocortisone ointment to the affected area to help reduce inflammation."
Henry also recommends keeping your skin as dry as possible, prioritizing sweat-wicking or synthetic fabrics, and staying on top of your hydration levels. "If you’re dehydrated, your sweat will have more salt and less water," she notes. "More salt increases irritation and in turn makes your skin more sensitive. Lubrication is key, and Chamois Butt’r Anti-Chafe Cream and Body Glide Anti-Chafe Balm are both great product options in addition to petroleum jelly or even aloe vera."
Body Breakouts
What is it, and what causes it? Body breakouts (be it back, chest, bum, boobs, or even the arms) are caused by the same factors that lead to breakouts on the face and, according to Henry, affect up to 50 million Americans yearly. As Zeichner explains, our skin naturally produces oil, and breakouts are triggered when said oil gets trapped by sticky skin cells that block the pores. In turn, levels of acne-causing bacteria begin to surge, which then promotes inflammation.
"Symptoms of acne include pimples like whiteheads and blackheads, which are the most common," says Henry. "Other types include cysts, which are painful and beneath the surface of your skin, pustules (small red pimples with pus at tips), and papules (red, raised bumps)."
What makes it worse? Stress, diet, hormonal imbalances, and heavy hair or makeup products can trigger breakouts, but according to Zeichner, body acne is especially prevalent during the summer months when we're sweating more and when our sweat is also more likely to mingle with higher ratios of dirt, oil, sand, and constrictive or wet clothing like swimsuits. Oh, and if you're working out and not changing or showering almost immediately afterward, that can also cause issues.

How to deal: "Change out of sweaty clothes and wash the skin immediately after working out," directs Zeichner. "Consider a benzoyl peroxide–containing cleanser to lower levels of acne-causing bacteria on the skin, and use it as a short contact therapy treatment. It needs to sit on the skin long enough to penetrate into the skin and do its job. A good rule of thumb is to let it sit as you sing the alphabet, and then rinse."
GlamDerm physician Elyse M. Love, MD, specifically recommends PanOxyl, which is a benzoyl peroxide body wash that's especially effective for helping to treat or manage body breakouts. However, since benzoyl peroxide can bleach clothing, make sure to thoroughly rinse and towel off before getting dressed.
Last but not lease, Zeichner says topical retinoids—which act like "pipe cleaners"—can also help keep pores clean. "Prescriptions like Altreno lotion, which you can get from a dermatologist, are specially formulated to minimize skin irritation, giving the benefits you expect from tretinoin." Just be sure to be extra diligent about your sunscreen application since topical retinoids increase skin sensitivity to sun exposure.
Maskne
What is it, and what causes it? As Love explains, "maskne" is typical acne that is caused or intensified by wearing a mask. Typically, she says you can expect maskne to present as red, inflammatory papules or whiteheads and clogged pores.
What makes it worse? According to Zeichner, there are two driving forces when it comes to maskne. First, the direct friction of wearing a mask against the skin causes inflammation around the follicles—a well-known phenomenon called acne mechanica that's common among athletes who regularly wear sports gear like helmets. Second, face masks trap sweat, oil, and dirt on the skin, which blocks pores and leads to breakouts. Therefore, it's important to try to keep the skin as clean and as clear as possible both before and after wearing a mask.

How to deal: In addition to washing your face before and after wearing a mask, forgoing makeup (if possible); making sure your mask is clean (Zeichner recommends dye-free, fragrance-free detergents such as Tide Free and Gentle, $13, to minimize potential irritation); and using skincare products containing AHAs, BHAs, or benzoyl peroxide are also strategic maskne antidotes. According to Love, products containing both of the aforementioned types of acids are excellent for the treatment of whiteheads, while products containing benzoyl peroxide are typically best for treating red, inflammatory papules.
"Beta hydroxy acid (salicylic acid) is a go-to ingredient to remove dead cells and extra oil from the surface of the skin to keep the pores clear," notes Zeichner. He particularly recommends InnBeauty Project's Foam Around Clarifying Daily Cleanse, which combines salicylic acid with an alpha hydroxy acid blend to gently exfoliate without overly drying out the skin. Then, after cleansing, he recommends applying a moisturizer to keep your skin barrier as healthy as possible. Prioritize formulas that contain soothing, calming, and strengthening ingredients such as niacinamide or peptides.
Folliculitis
What is it, and what causes it? "Folliculitis is an infection of the hair follicles, usually caused by staph bacteria," explains Zeichner. "It usually looks like red bump and pus pimples surrounding hair follicles and often occurs on the neck, chest, back, and buttocks. It usually develops when the skin barrier becomes disrupted, increasing the risk of bacteria infecting the skin, and can also occur where hair has been removed."
What makes it worse? According to Zeichner, waxing or shaving causes microscopic damage to the outer skin layer, which in turn increases the risk of skin infection. However, folliculitis can be tricky to identify and diagnose since it is commonly mistaken for acne.

How to deal: Mild versions of folliculitis will typically go away on their own, but as both Henry and Zeichner share, the condition can also be treated with either topical or oral antibiotics prescribed from your dermatologists, or OTC antimicrobial skin cleansers like this one from Hibiclens can help kill off bacteria hanging out on the skin. Zeichner notes that acne cleansers containing benzoyl peroxide such as Clean and Clear's Continuous Control Cleanser can also lend a helping hand to eradicate bacteria. Henry also recommends steroid cream and warm saltwater compresses.
"If symptoms don’t resolve within one to two weeks or become painful at any time, you should consult your physician," says Henry. "You don’t want to leave an infection unchecked."
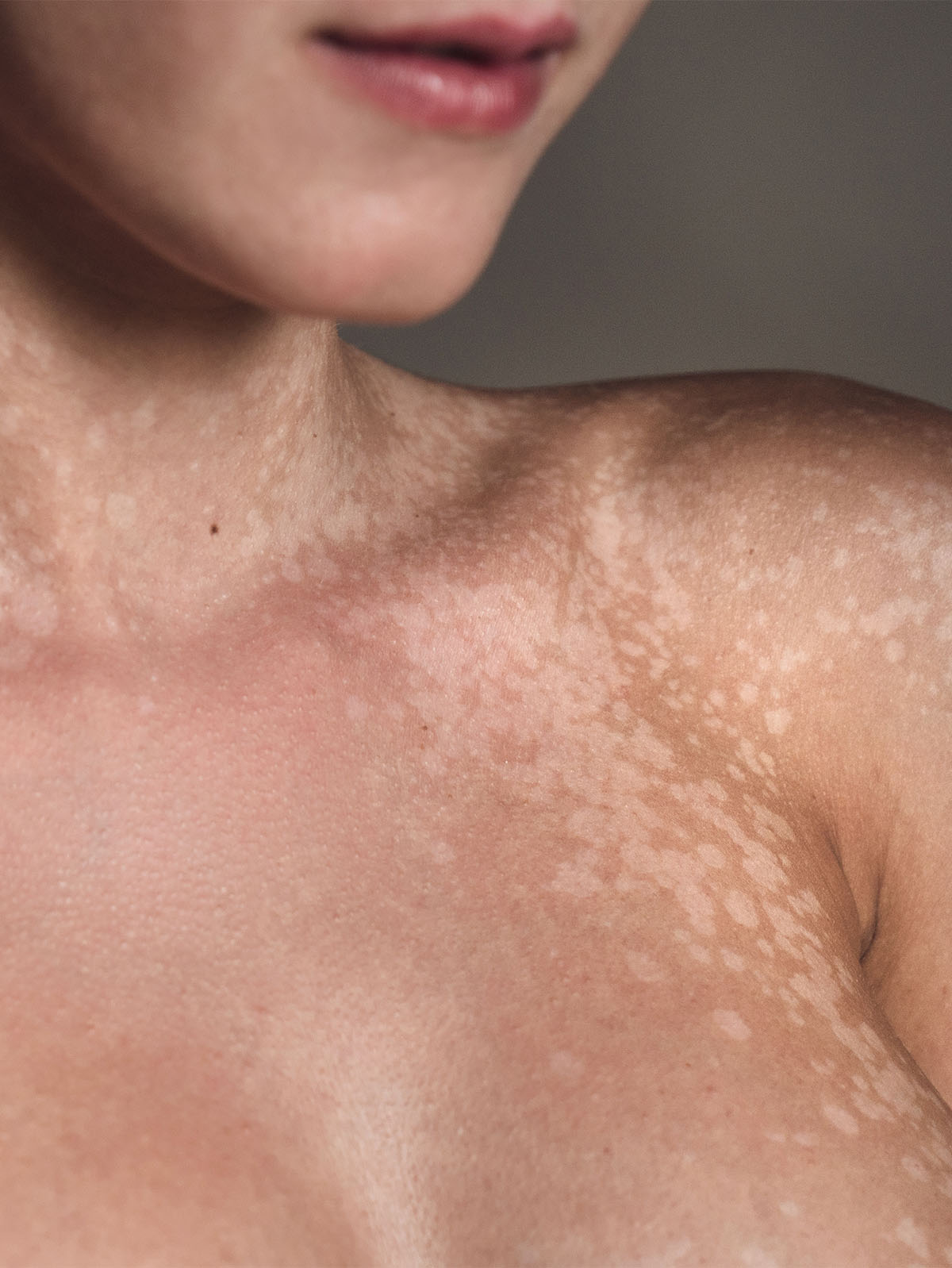
Melasma
What is it, and what causes it? "Melasma is a skin condition where dark, discolored patches appear on the skin and mainly on the face—especially the bridge of the nose, cheeks, upper lips, forehead, neck, even the arms," Henry shares. "It most commonly affects pregnant women, and it’s much more common in women than it is for men." In addition to pregnancy, Henry says other potential causes or triggers for melasma include hormonal changes or fluctuations stemming from birth control, exposure to the sun, and thyroid disease.
What makes it worse? Exposure to the sun—make sure to use a good SPF daily! Henry is a fan of Neutrogena's Ultra Sheer Dry-Touch Sunscreen SPF 100, which she says is a great choice for maximum protection.

How to deal: First things first: While Henry confirms at-home treatments might indeed be effective treatment options during the early stages of melasma, you'll want to work with a dermatologist to devise an action treatment plan if you're in the later stages.
That said, to help treat and manage melasma, Henry recommends (again) staying out of the sun, wearing a 30-or-higher SPF sunscreen whenever you're outside for more than an hour, taking tranexamic acid orally, and/or trying a lotion or gel containing hydroquinone, which can help lighten skin patches. She specifically recommends Glytone's Dark Spot Corrector With 2% Hydroquinone + Kojic Acid.
Keratosis Pilaris
What is it, and what causes it? Zeichner explains keratosis pilaris, commonly known as KP, as the buildup of dead cells within hair follicles. Often located on the outside of the arms or on the thighs and bum, KP looks like red, rough pinpoint bumps. "Roughly 50% to 80% of American adolescents experience KP, and roughly 40% of adults," Henry tells us. "It’s one of the most common skin conditions."
What makes it worse? "KP is caused by a buildup of keratin, a protein that makes up the tissues of your skin and protects your body from infection," says Henry. "Dry skin and eczema may contribute to this buildup, but researchers aren’t sure exactly what causes it. It also becomes worse in colder weather and if you have dry skin." Like most skin conditions, touching and picking will likely make KP worse, so try to stay as hands-off as possible.
How to deal: In addition to resisting the temptation to pick and touch, incorporating effective exfoliating moisturizers into your routine is a gentle, skin-friendly way to help remove accumulated dead cells from the skin. "CeraVe's Salicylic Acid Lotion hydrates the skin and helps exfoliate dead skin cell buildup to improve KP's signature rough bumps," says Zeichner. That said, since KP is hereditary, there isn't a full-on cure, and you'll need to rely on thick moisturizers and gentle skincare formulations to help manage the condition. Henry also recommends humidifiers to maintain your skin's hydration levels and to keep your showers short, avoiding hot water.
Cold Sores
What is it, and what causes it? Also known as "the kissing disease," cold sores usually develop around the mouth and are caused by a virus called HSV, which Zeichner says is spread through direct, person-to-person contact. "Patients with cold sores develop painful, grouped blisters on or around the lip area, and once infected, the virus takes up residency within the nerves and will pop up via a visible cold sore outbreak when you are run-down or have a compromised immune system," he says.
What makes it worse? In addition to the aforementioned weakened immune system, sunburns, spicy foods, fever, or trauma to the lips can also trigger a cold sore.

How to deal: As far as managing the condition, Zeichner recommends topical or oral antiviral medications such as Abreva, which you can get OTC. Additionally, since cold sores are highly contagious, Zeichner says to avoid kissing during an outbreak so you don't spread the virus.
Psoriasis
What is it, and what causes it? "Psoriasis is a non-contagious skin condition where the immune system essentially gets angry at the skin, which in turn leads to inflammation," Zeichner tells us. "Patients develop red, scaly plaques that typically develop on the elbows and knees but can occur anywhere on the body." Essentially, Henry explains, the skin builds up and cells multiply up to 10 times faster than they normally would. More than eight million Americans suffer from the condition. "Psoriasis is an autoimmune condition, and you’ll want to be careful about identifying and avoiding your triggers," she warns.
What makes it worse? Genetics, hormonal changes, lifestyle habits such as drinking alcohol and smoking, stress, medications, intense sun exposure, and infections can all cause or make psoriasis worse.

How to deal: According to Zeichner, mild cases can be treated with topicals like moisturizers and anti-inflammatory creams, but for severe cases, you may need to see a dermatologist, who might recommend or prescribe oral or injected medications to help manage the condition.
For at-home care, stick to moisturizers containing ingredients like petrolatum, which help soften scale buildup. Zeichner specifically recommends Vaseline Intensive Care Advanced Repair Lotion, which contains triple-purified petrolatum to protect the skin with a non-greasy finish that easily spreads and absorbs into the skin once applied. Additionally, Henry says daily exposure to sunlight (just don't overdo it, and wear sunscreen!), keeping a humidifier in your bedroom, and avoiding your triggers (she suggests keeping a diary to help) can also be beneficial when managing psoriasis.
Eczema
What is it, and what causes it? "Eczema is a term for a group of conditions that cause itchy, cracked, inflamed, and rough skin, and it affects 10% to 20% of infants and about 3% of children and adults," Henry tells us.
For the most part, genetic and environmental triggers are to blame, and as far as symptoms, she recommends looking out for dry, sensitive skin that may be itchy, in addition to rough, leathery patches of skin, swelling, and inflamed skin in tones of red, purple, or gray.
What makes it worse? Everyday allergens like pollen, mold, and pet dander can trigger an eczema flare alongside weather since both extreme cold and hot temperatures can aggravate the condition.

How to deal: If you have eczema, it's a good idea to consult your physician. Henry explains that your doctor might prescribe specific ointments with corticosteroids to calm inflammation or oral immunosuppressants. For at-home management, she recommends keeping the skin clean and well-moisturized. So daily showers or baths and topping up your skin with calming lotions or creams is a must. (She recommends both of these options from Vaseline and Avène.)
"If you can’t get your eczema under control, try to choose hydrating cleansers in addition to hypoallergenic laundry detergent—they're less likely to further irritate your skin," she adds.

Erin has been writing a mix of beauty and wellness content for Who What Wear for over five years. Prior to that, she spent two and half years writing for Byrdie. She now calls Santa Monica home but grew up in Minnetonka, Minnesota, and studied writing, rhetoric, and communication at University of Wisconsin, La Crosse. She studied abroad in Galway, Ireland, and spent a summer in L.A. interning with the Byrdie and Who What Wear family. After graduating from UW, she spent one year in San Francisco, where she worked as a writer for Pottery Barn Kids and PBteen before moving down to L.A. to begin her career as a beauty editor.












